Lymphatic Drainage Massage: A Vital Tool for Post-Surgery Recovery
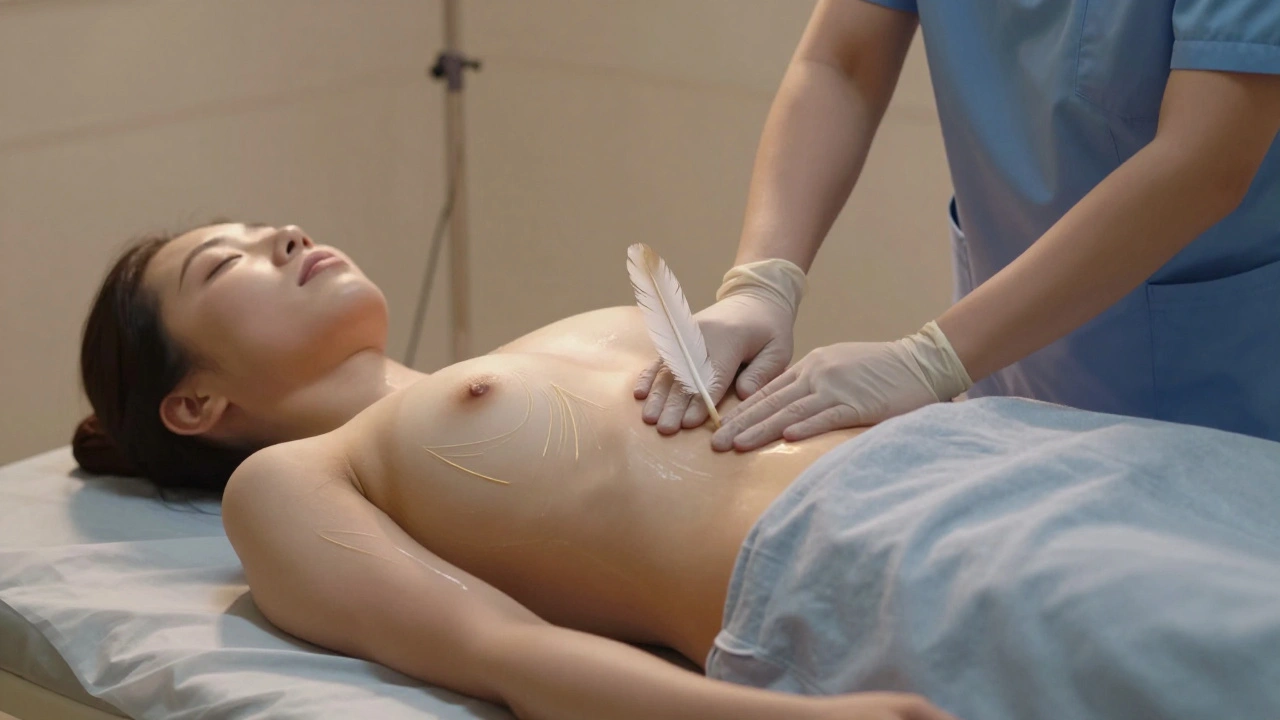
After surgery, your body doesn’t just need rest-it needs help moving fluid. Swelling, stiffness, and slow healing aren’t just normal side effects. They’re signs your lymphatic system is overwhelmed. That’s where lymphatic drainage massage comes in. It’s not a luxury. It’s a critical part of recovery for many patients after procedures like liposuction, mastectomy, tummy tucks, or even knee replacements.
What Happens to Your Lymphatic System After Surgery?
Your lymphatic system is like a cleanup crew. It drains excess fluid, filters out waste, and fights infection. But surgery? It’s like shutting down a highway. Scar tissue forms. Lymph nodes get removed. Fluid gets stuck. That’s when swelling doesn’t go away after a few days-it lingers for weeks. Patients often describe it as feeling heavy, tight, or even numb in the affected area. Some notice their clothes don’t fit the same way. Others feel fatigued even after sleeping well.
Without proper drainage, this fluid turns into fibrosis-thick, fibrous tissue that’s hard to reverse. That’s why recovery isn’t just about healing the incision. It’s about restoring flow. And that’s where manual lymphatic drainage (MLD) makes a real difference.
How Lymphatic Drainage Massage Works
Unlike deep tissue or sports massage, lymphatic drainage is incredibly light. Think feather-light pressure-like gently brushing the surface of a peach. The goal isn’t to push fluid out. It’s to guide it. Therapists use slow, rhythmic strokes that follow the natural pathways of lymph vessels. These movements encourage fluid to move toward healthy lymph nodes that are still working.
It’s not about muscle tension. It’s about direction. A single session can move hundreds of milliliters of fluid that would otherwise sit in your tissues. Studies from the Journal of Plastic and Reconstructive Surgery show patients who received daily MLD after breast cancer surgery had 40% less swelling at six weeks compared to those who didn’t. That’s not minor. That’s life-changing.
Who Benefits the Most?
Not everyone needs it-but many do. Here’s who sees the biggest results:
- Patients after liposuction or body contouring
- Those who had lymph nodes removed (common in breast, pelvic, or melanoma surgeries)
- People recovering from major abdominal or orthopedic surgeries
- Anyone with persistent swelling beyond two weeks post-op
Even if you didn’t have lymph nodes removed, scar tissue can block flow. A tummy tuck creates layers of scar tissue under the skin. That’s a natural barrier to lymph movement. MLD helps soften that tissue before it hardens.
When to Start-And When to Wait
You can’t rush this. Timing matters. Start too early, and you risk disrupting healing. Wait too long, and fibrosis sets in.
Most surgeons recommend waiting until the first follow-up-usually 5 to 10 days after surgery. That’s when the initial bleeding and inflammation have settled, but before scar tissue hardens. Some patients begin as early as day 3 if their incisions are stable and their doctor approves.
It’s not a one-time fix. Most patients need 5 to 10 sessions over 2 to 4 weeks. Some, especially after cancer surgery, continue for months. Think of it like physical therapy for your fluid.
What to Expect During a Session
First, you’ll lie down on a table, usually on your back. The room is warm and quiet. The therapist uses clean, gloved hands and moves slowly. You might feel a gentle pulling sensation-not pain, not pressure. Some people fall asleep. Others feel warmth spreading through the area.
Sessions last 45 to 75 minutes. You won’t feel sore afterward. In fact, many report feeling lighter, calmer, and more energized. That’s because your body isn’t fighting fluid buildup anymore. Your immune system can focus on healing.
What Doesn’t Work
Not all massages are created equal. Avoid deep pressure, hot stones, or aggressive kneading. Those can damage fragile tissue or push fluid into areas that can’t drain. Even compression garments alone aren’t enough. They help, but they don’t stimulate flow. They’re a support, not a solution.
And skip the DIY videos. YouTube tutorials often show techniques that are too forceful. You need trained hands. A certified lymphatic therapist knows where the nodes are, how the vessels run, and how to adjust for your specific surgery.
Real Results, Real Stories
One patient, after a double mastectomy with reconstruction, had swelling so severe she couldn’t wear a bra for six weeks. After five MLD sessions, she was able to wear a soft camisole. Another, who had a tummy tuck, noticed his stomach felt softer and flatter after just three sessions. He didn’t lose weight-he just stopped holding onto fluid.
These aren’t outliers. They’re the norm for patients who get consistent care. The difference isn’t magic. It’s science. Lymphatic drainage massage reduces inflammation, speeds up healing, and prevents long-term complications like chronic swelling or lymphedema.

How to Find the Right Therapist
Look for someone certified in Complete Decongestive Therapy (CDT) or Manual Lymphatic Drainage. Ask if they’ve worked with post-surgical patients before. A good therapist will ask about your surgery, your doctor’s recommendations, and your current symptoms. They won’t push you into a package. They’ll tailor the plan.
Most clinics offer a free 15-minute consultation. Use it. Ask how many post-op patients they see each month. If they say ‘a few,’ keep looking. If they say ‘10 to 20,’ you’re on the right track.
Can You Do It Yourself?
After your first few sessions, your therapist may teach you gentle self-massage techniques. These are for maintenance-not replacement. You can do them daily at home: light strokes toward your collarbone, under your arms, or along your inner thighs, depending on your surgery site. But don’t try to replace professional sessions. The depth and precision matter.
Why This Isn’t Just About Swelling
Reducing swelling is the visible benefit. But the deeper win? Your immune system wakes up. Lymph carries white blood cells. When fluid stagnates, infection risk goes up. Healing slows. Fatigue lingers.
After MLD, many patients report better sleep, less pain, and even improved mood. Why? Because their body isn’t stuck in recovery mode. It’s moving forward.
This isn’t a fringe therapy. It’s standard care in Europe and parts of Asia. In the U.S., it’s growing fast-not because of trends, but because patients are demanding better outcomes. And the data backs it up.
If you’re recovering from surgery and still feeling swollen, stiff, or tired after two weeks, don’t just wait it out. Talk to your surgeon about lymphatic drainage massage. It might be the missing piece in your recovery.


